New research published by the Journal of the American Medical Association (JAMA) estimates that 25% of U.S. healthcare spending, or $760 billion to $935 billion, is spent annually on waste1. According to the study, the greatest source of healthcare waste is administrative complexity, which accounts for $265.6 billion in annual waste.
Part of this administrative burden stems from a complex claims adjudication process impacted by legacy or outdated technology, a lack of clear contract or policy information, and no universal way for sharing information (e.g., member’s name, diagnosis code, etc.). These administrative challenges results in data and eligibility errors that are made throughout the claims continuum, resulting in millions of dollars in improper payments.
Life of a claim: Errors along the way
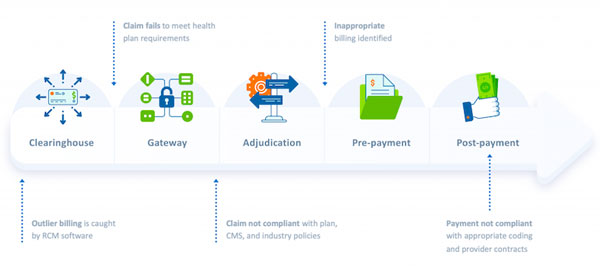
Despite the best efforts to address waste, administrative complexity in the healthcare system continues. Recent research from JAMA shows that measures to eliminate healthcare waste would result in a 25% improvement, but there’s more work to be done. Finding the root causes of errors is the most effective way to ultimately remove waste—and the high cost of it—from health plans’ payment integrity operations.
Here are three approaches to combatting the high cost of waste in your payment integrity strategy.
1. Reduce manual processes
Manual processes are often at the heart of human error. Manual processes are tedious, error-prone, and inefficient, contributing to the high cost of waste in healthcare. When your entire claims adjudication or payment integrity process contains manual tasks, the likelihood of error is high. Reducing or eliminating manual effort in your payment integrity processes will go a long way toward reducing waste.
2. Use technology to your advantage
Technology plays a key role in taking out waste from the payment integrity process. But outdated or legacy technology can create just as much waste as you might find with manual processes. With the right technology in place, you can modernize your payment integrity processes and reduce the amount of time and effort associated with correcting complex claims.
By the same token, emerging technologies like artificial intelligence and machine learning solve traditional payment integrity problems in new and innovative ways. These technologies offer analytics and predictive insights that can optimize your claims payment processes and drive data-driven decisions.
3. Look to a partner for advanced capabilities
A partner can supplement your in-house operations and offer the expertise you need to reduce waste. The right partner will bring robust capabilities that round out your core operations—capabilities like data mining techniques that prevent incorrect and unnecessary payments; industry experts who are up on the ever-changing and complex healthcare landscape; and processes that identify opportunities to correct, recover, and prevent improper payments at all points in the claims’ lifecycle.
The high cost of waste can threaten the viability of organizations throughout the healthcare ecosystem. With a holistic, connected payment integrity strategy built around these three tenets, your organization can improve operational efficiencies and achieve financial integrity by preventing improper payments—all while eliminating waste and generating meaningful results.
To learn how MultiPlan can help you advance into the future of payment integrity, contact us today.
1 “Waste in the US Health Care System: Estimate Costs and Potential for Savings,” JAMA, October 7, 2019.
Previously published on the former Discovery Health Partners website.

